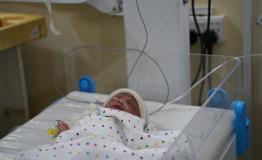
Mudug region in Somalia, is hosting approximately 151,000 internally displaced people as drought-driven displacement continues across the region. Funding cuts have forced dozens of health and nutrition sites to close, water sources have dried up, and malnutrition admissions at MSF facilities surged sharply in 2025. Frauke Ossig, MSF's Operational Manager for Somalia, recently returned from a field visit to Mudug. She explains what she saw — and what it will mean for patients if the response does not change.
Mudug is hosting over 150,000 displaced people. What is the reality families are living through right now?
Mudug is on the edge. Families arrive in displacement sites after walking enormous distances, having already exhausted every option they had. Many wells have dried up entirely — by December 2025, authorities reported 71 non-functional boreholes and wells across Galgaduud and Mudug — and water prices have more than doubled. Families are making impossible choices between buying water, food, or the cost of transport to reach a clinic.
When patients finally arrive at our facilities, we can see in their condition exactly how long they waited. The crisis does not start at our door. It starts kilometres away, in a village with no clean water and no functioning health post. And an early-warning alert in December 2025 reported that another 29,142 people had been displaced across Bari, Mudug, Nugaal, and Sanaag — which means the pressure on already-stretched communities is not easing. It is growing.
What are MSF teams seeing medically — and what does that tell you about what is happening outside your facilities?
The numbers are stark, but they represent real children. In 2025, MSF recorded approximately 117,840 outpatient consultations and 56,444 emergency consultations in Mudug. Malnutrition admissions surged — a 46 percent increase in outpatient cases and a 58 percent rise in inpatient cases compared to 2024. More than 3,800 children were enrolled in ambulatory therapeutic feeding centres, and 2,200 required inpatient care. We also treated over 56,000 respiratory infections, nearly 16,000 cases of acute watery diarrhoea, and 801 measles cases.
By the time patients reach our clinics, they have already walked long distances and exhausted every option. What we see inside our facilities is a reflection of what is failing outside them.Frauke Ossig, MSF Operational Manager for Somalia
These figures are a mirror. They tell us that safe water, nutrition, and vaccination are failing outside our walls — and that illnesses which should be manageable are becoming life-threatening because families cannot reach care in time.
Dozens of health and nutrition sites have closed due to funding cuts. What does that mean for a family trying to get help?
It means there is simply nowhere left to go. When first-line services close, people do not stop being sick — they delay care until the illness becomes critical. Funding reductions have forced dozens of health and nutrition sites in Puntland alone to close or face severe staff and supply shortages. Antenatal and postnatal visits dropped in 2025 despite rising needs. Referral options for complicated cases are shrinking.
Nationally, at least 4.4 million people faced high levels of acute food insecurity in late 2025, and 1.85 million children under five are projected to suffer acute malnutrition between August 2025 and July 2026 — including 421,000 severe cases. MSF can provide essential services: outpatient care, emergency treatment, maternal health, vaccination, and mobile clinics reaching displacement sites and remote villages. But MSF cannot replace a collapsing system.
When first-line malnutrition treatment and basic primary healthcare shrink, patients face longer journeys and higher costs, increasing the likelihood of late presentation and preventable deaths.Frauke Ossig, MSF Operational Manager for Somalia
What needs to happen now — and what is the cost of waiting?
We are calling on donors and humanitarian actors to take three urgent steps. First, sustain and scale up integrated health and nutrition services close to where people live. Predictable funding prevents site closures and enables early treatment — the single most effective way to reduce complications and deaths. Second, reinforce routine vaccination and outreach so that preventable diseases like measles do not spread further in already weakened communities. Third, invest in safe water and sanitation — repair wells and expand water trucking — to reduce diarrhoeal disease and support nutrition gains.
Our 2025 data already shows a system under severe strain. Without a course correction now, 2026 will be worse.Frauke Ossig, MSF Operational Manager for Somalia
If these steps are delayed, the trajectory is clear: displacement will continue, more children will arrive in critical condition, outbreaks will spread, and preventable deaths will rise. There is still time to act — but the window is narrowing.